Article Text
Abstract
Background In 2019, ever-smoking prevalence among adults in Indonesia was 32.8%, which may correlate with a high burden on the economy. Therefore, there is an urgent need to estimate the economic costs of tobacco use, which are crucial for policymakers in planning healthcare provisions and other public expenditures.
Methods We follow the WHO standard approach, multiplying the sum of the direct and indirect costs with the smoking-attributable fraction. Direct costs include healthcare and non-healthcare costs. Indirect costs include the loss of productivity resulting from absence from work and premature death due to smoking-related illnesses.
Findings We found that the 2019 economic cost of smoking ranges from Rp 184.36 trillion to Rp 410.76 trillion (1.16%–2.59% of the gross domestic product). This research found a similar economic cost of smoking compared with a previous estimate conducted by Kosen et al of Rp 438.5 trillion. However, the estimated direct cost of smoking ranges from Rp 17.9 trillion to Rp 27.7 trillion, which is higher than the estimate of Rp 15.5 trillion by Kosen et al. Badan Penyelenggara Jaminan Sosial Kesehatan allocated between Rp 10.4 trillion and Rp 15.6 trillion to cover the healthcare costs attributable to smoking, representing between 61.2% and 91.8% of the 2019 deficit.
Conclusions The vast economic cost of smoking is a waste of resources and a burden on Indonesia’s National Health Insurance System. Therefore, the government must increase cigarette taxes to correct the negative externalities of smoking consumption.
- economics
- smoking caused disease
- public policy
Data availability statement
Data are available on reasonable request.
Statistics from Altmetric.com
Introduction
By 2030, tobacco use will be the leading cause of premature deaths and disability among adults worldwide,1 generating significant economic burdens on health systems and other social institutions,2 especially in low-income and middle-income countries (LMICs). Globally, annual tobacco-related deaths are projected to rise from 6.4 million in 2015 to 8.3 million in 2030,3 with 80% of deaths occurring in LMICs.4
Indonesia’s tobacco use epidemic remains one of the world’s most serious. Based on the 2019 National Socio-Economic Survey (Survei Sosial-Ekonomi Nasional (SUSENAS)), the prevalence of adult ever-smoking in 2019 was 32.8%, where the prevalence of ever-smoking among Indonesian adult males reached 64.5%. The prevalence of ever-smoking among children is also increasing. Ever-smoking prevalence among children aged 10–18 increased from 7.2% in 20135 to 9.1% in 2018.6 About 51.3% of all adults7 and 66.2% of youth aged 13–15 are regularly exposed to secondhand smoke.8
The National Medium-Term Development Plan (Rencana Pembangunan Jangka Menengah Nasional) 2020–2024 recognises smoking as a threat to the national development agenda.6 Smoking lowers the effectiveness of social protection programmes9 and overburdens the health system.10 The top five leading causes of premature deaths in Indonesia are tobacco-related and cause about 16.2% of total deaths (24.3% of adult male deaths; 6.3% of adult female deaths).11 Three of these diseases dominate National Health Insurance System (Jaminan Kesehatan Nasional (JKN)) claims.12 The previous study by Kosen et al 10 estimated that the total cost of smoking in Indonesia is around Rp 438.5 trillion (at the 2019 value). They also found that the direct cost of smoking for accessing healthcare treatment was only Rp 14.2 trillion (or Rp 15.5 trillion at the 2019 value), lower than the official figures published by the Social Security Agency for Health (Badan Penyelenggara Jaminan Sosial Kesehatan (BPJS-K)) at Rp 25.1 trillion.
The objective of this study is twofold. First, it intends to re-estimate the direct and indirect cost of smoking in Indonesia using the WHO standard approach13 to complement a study conducted by Kosen et al.10 They estimated the direct and indirect cost of smoking based on 33 diseases attributable to tobacco use, such as cancer, cardiovascular diseases and respiratory diseases. While the direct healthcare costs of smoking were estimated from direct health expenditures on treatment, Kosen et al employed disability-adjusted life years (DALYs) to estimate the indirect cost of smoking in Indonesia.
Second, this study aims to estimate the burden of the direct cost of smoking to JKN based on all disease types. These findings will emphasise that reducing the cost of smoking-attributable diseases would significantly impact the sustainability of JKN in the short term. In the longer term, implementing tobacco control through cigarette taxation might discourage smoking behaviour, leading to negative externalities.
Data and methodology
This study follows the standard approach of WHO,13 which multiplies the sum of the direct and indirect costs of smoking with the smoking-attributable fraction (SAF). The analytical model uses four sources: Statistics Indonesia (BPS), Ministry of Health (MoH), administrative data from the BPJS-K and additional information for the macroeconomic figures from the World Development Indicators (WDI). The 2019 BPJS-K administrative data present direct healthcare costs for inpatient and outpatient medical treatment that is disaggregated by gender and age group. The out of pocket (OOP) of uncovered medical costs by BPJS-K, medical treatments and transportation costs for seeking medical treatment is estimated using SUSENAS.
SUSENAS is a regular survey conducted in March and September every year by BPS. The March survey collects information from 320 000 households, which equals 1.2 million individuals, representing the total population of Indonesia. SUSENAS is divided into two modules. The first module is the demographic module that captures information on individual and household characteristics, such as age, gender, level of education, access to health facilities and household assets. The second module refers to household consumption, which is divided into two main blocks: (1) food block recording 188 items of food, beverage and tobacco on a weekly basis, and (2) the non-food block collecting information of 122 items on either a monthly basis or an annual basis.
In the case of health expenditure, SUSENAS distinguishes OOP healthcare expenditures from the total healthcare expenditures, which include access to healthcare treatment at different types of healthcare facilities, pharmaceutical costs and other health-associated costs. While outpatient visits were recorded monthly, the number of inpatient visits was requested over the past 12 months. The 2019 SUSENAS also gave detailed information on cigarette consumption and quantity per household. Online supplemental appendix 1 shows the detailed information of the 2019 SUSENAS.
Supplemental material
The Indonesia Basic Health Research 2018 (Riset Kesehatan Dasar (RISKESDAS)), published by MoH, presents information on the age at which smoking is initiated. The 2019 Indonesia Life Table and the 2019 National Labor Force Survey (Survey Tenaga Kerja Nasional) are published by BPS, and the gross national income (GNI) and gross domestic product (GDP) numbers obtained from WDI are used to estimating future loss due to premature death (ie, indirect mortality cost).
Relative risk
Since the relative risk (RR) of smoking for Indonesia is not available and the data do not provide consistent estimates, this study uses RRs from other countries to calculate the SAF for Indonesia. To provide a range of estimates for the cost of smoking, this study uses RRs from India and the USA. The RR from India was used because of the similarity to Indonesia in demographic characteristics, lifestyle and smoking intensity. The RR from India may also reflect similar patterns in Indonesia to accessing healthcare. However, since RR for illness due to smoking in India is not available, the RR of death due to smoking is used. Our study strongly assumed that it is not much difference between the RR of morbidity and mortality. Meanwhile, the RR from the USA was used as an alternative estimate that can be used to compare and provide a range of estimations. Unlike the RR from India, the RR from the USA represents the risk for illness smokers face in the country.
The US Department of Health and Human Services14 presents the RR for US individuals aged 35 years and above, disaggregated by gender and age group. Moreover, the RR distinguished between current smokers and former smokers. Since this study estimates the economic cost of smoking for ever-smokers, the average RR for current and former smokers is applied. However, since the reported RR in the USA is only available starting at age 35 years, we used this number to calculate SAF for individuals younger than 35 years. We then estimated the SAF by multiplying the RR with the ever-smoking prevalence for each age group and gender.
The RR from India was adopted from Jha et al,15 which captures individuals aged 30–69 years, comparing ever-smokers with never-smokers within the last 5 years, with separate RRs for men and women. The survey asked a respondent (typically a household member) if the deceased person had been a smoker within the last 5 years and, if so, how many the usual number of beedi and/or cigarettes are consumed per day. We encountered a similar limitation as with the RR from the USA, where the RR from India captures the risk starting at age 30 years (and above). Therefore, to estimate the fraction of diseases attributable to smoking for individuals between the ages of 20 and 30 years in Indonesia, we applied India’s RR for age 30 years.
Despite using two RRs, the RR from India served as the benchmark for our estimation because of the similar prevalence of ever-smoking individuals. While Indonesia reported a 32.8% prevalence of ever-smoking based on the 2019 SUSENAS, India reported that 29% of adults are tobacco users. The difference between Indonesia and India comes in the form of tobacco being consumed. Most of the tobacco consumption in Indonesia is in the form of cigarettes, while most of the tobacco consumption in India is smokeless tobacco. The RR from the USA then served as an alternative estimation. We noted that the RR of the USA may result in an overestimation of the cost of smoking, while the RR of India may underestimate the cost of smoking. An underestimation comes from the RR of mortality that may be lower than the RR of morbidity. In contrast, overestimation comes from the RR of morbidity in the USA that may be higher than the case of Indonesia. However, many studies have shown no significantly impact on using such estimates.16–18 Therefore, the use of two RRs will provide an interval estimate of economic cost of smoking in Indonesia.
The economic burden of smoking
The term ‘economic burden’ is defined as the difference between healthcare or other economic costs incurred due to smoking, and the costs that would have been incurred had the individual not smoked.13 Based on the conventional cost of illness approach, the economic consequences of illness are divided into three components: (1) direct cost including healthcare costs (eg, inpatient medical treatment, general practitioners and other service fees, medical supplies, medicines, etc) and non-healthcare costs (eg, transportation to health facilities); (2) indirect morbidity cost, which includes productivity loss due to an individual’s illness; (3) indirect premature mortality cost, which refers to economic loss due to an individual’s premature death.
The economic costs (EC) may be expressed as follows:
 (1)
(1)
 (2)
(2)
Here, SDE is smoking direct expenditures; SMIE is smoking indirect expenditures; SAIMbC is smoking-attributable indirect morbidity costs; SAIMtC is smoking-attributable indirect mortality costs; i is age group and l is the number of age group.
Estimating the SDE
This study estimates the cost for all aged populations and all individuals aged 20 years and older. Smoking behaviour affects health outcomes in three stages, that is, immediate, intermediate and long-term effects.19 While the immediate effect of smoking can be observed as soon as individuals start to smoke, the intermediate and long-term effects are observed once the individuals consume tobacco after some period. Bonnie et al 19 identified that the intermediate effects could be observed in young adulthood, while the long-term effects are present once individuals enter older phases of life. Therefore, this study assumes a 10-year latency period, as the smoking initiation in Indonesia occurs as early as 10 years old.20
SDE represents the medical expenses incurred by individuals and health insurance providers to access healthcare treatment. SDE includes direct healthcare expenditures (DHE) and direct non-healthcare expenditures (DNHE). DHE includes both OOP and health insurance provider expenditures for inpatient care at public and private hospitals, outpatient care at primary health facilities, payments of fees to private general practitioners and traditional healers and medical expenditures for medicine that patients purchase themselves, including prescriptions and over-the-counter drugs.
DNHE includes transportation costs paid by individuals to access healthcare. Direct non-health care expenditures might include transportation for caregivers and lodging and food expenditures for more than one caregiver. In the absence of reliable data for these elements, our calculation might be underestimated. We estimated the transportation cost using the 2018 SUSENAS and adjusted for inflation to get the 2019 value due to inconsistent questions in the 2019 SUSENAS compared with other SUSENAS.
To calculate the DHE and DNHE, we used 2019 SUSENAS that captures the OOP expenditures to access health treatment by facility type and treatment type (ie, inpatient vs outpatient). The 2019 SUSENAS also presents information on non-health expenditures, such as transportation costs to the health facilities where treatment is needed. Furthermore, the aggregated administrative data by gender and age group on annual claims for inpatient treatment and outpatient visits are directly obtained from BPJS-K data. The aggregated administrative data on claims paid by BPJS-K are representative of the 2019 fiscal year.
Unlike the previous study conducted by Kosen et al,10 which captured only 33 types of illnesses, we assume that smoking habits will cause more health issues, from minor illnesses to more serious diseases. Our assumption follows findings from the US Department of Health and Human Services,14 which found a direct relationship between smoking behaviour and minor illnesses, such as tooth decay, type 2 diabetes and even diseases caused by bacterial infections. Thus, we rely on the SAF estimated from the relative risk of smoking to capture the possible diseases faced and subsequent treatment needed by ever-smoking individuals.
Next, the SAF is calculated and used for estimating SDE as:
 (3)
(3)
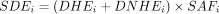 (4)
(4)
Here, ESMOKE is an ever-smoking prevalence of the population (%) that is drawn from the 2019 SUSENAS; RR is referring to the India’s RR and the US’s RR; DHE is smoking direct healthcare expenditures and DNHE is direct non-healthcare expenditures.
Smoking indirect expenditures
Indirect morbidity costs (SAIMbC)
The SAIMbC quantifies how much the nation’s entire economy suffers from the loss of individual productivity during their illness (either during inpatient treatment or during unproductive days due to illness). The formula to calculate SAIMbC is as follows13:
 (5)
(5)
Here, Pop represents total population by age group; LFPR is the labour force participation rate, defined as the share of employed persons out of the total eligible labour force; W is the average daily income. Two measurements for daily income are used in this study, per capita GDP and per capita GNI.
However, this study does not use the wage data because it comes from respondents’ self-assessment, which may be inaccurate. In addition, two groups of workers, that is, unpaid domestic workers and those self-employed and assisted by non-paid workers, do not report any income in the survey, which implies that wage data may suffer from self-reporting bias that leads to underestimated figures. Therefore, to capture income generated from economic activity, this study employs GDP per capita and GNI per capita.
GDP per capita measures the income per capita generated by individuals who reside in Indonesia, regardless of their nationality. On the contrary, the GNI per capita presents the sum of a country’s GDP per capita plus net income (positive or negative) per capita from abroad. Since GNI per capita captures income from Indonesian migrant workers who resides in other countries, the direct healthcare costs of these workers will occur abroad and thus will not be captured in the JKN. Moreover, regardless of their nationality, all residents are required to register in the JKN programme, so their direct healthcare costs will be a part of JKN.21 Therefore, this study prefers to employ GDP per capita as the main indicator for income in the estimate and use the GNI per capita as an alternate indicator to provide an estimated range of the economic costs of smoking.
Indirect mortality costs (SAIMtC)
The SAIMtC measures economic loss due to premature death from smoking behaviour. First, we estimate the total number of premature deaths attributed to tobacco use (smoking-attributable mortality (SAMes)) as follows13:
 (6)
(6)
Here, POP is a population drawn from the 2019 SUSENAS, while Death is the death rate drawn from Indonesia’s life table. Second, we estimate the expected present value of future productivity lost for each of those deaths (PVLE) that follows13:
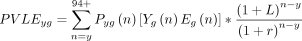 (7)
(7)
Here,  is a present discounted value of lifetime earnings for a person of age y and gender g;
is a present discounted value of lifetime earnings for a person of age y and gender g;  is the probability that a person of age y and gender g will survive to age n;
is the probability that a person of age y and gender g will survive to age n;  is the average annual earnings of an employed person for gender g and age n;
is the average annual earnings of an employed person for gender g and age n; 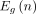 is the proportion of the population of gender g and age n that are employed in the labour market (LFPR); L is the rate of increase of labour productivity and r is the real discount rate. We then convert
is the proportion of the population of gender g and age n that are employed in the labour market (LFPR); L is the rate of increase of labour productivity and r is the real discount rate. We then convert  into
into 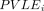 . Like the indirect morbidity cost, we used GDP per capita and GNI per capita as a proxy for the annual earnings of an employed person by gender and age group. Labour productivity is measured using the GDP growth rate, while the actual discount rate was the inflation rate in 2019.
. Like the indirect morbidity cost, we used GDP per capita and GNI per capita as a proxy for the annual earnings of an employed person by gender and age group. Labour productivity is measured using the GDP growth rate, while the actual discount rate was the inflation rate in 2019.
Once the PVLE and the SAMes were calculated, smoking-attributable mortality cost was calculated using formula as follows:
 (8)
(8)
Here, SAIMtC is the smoking-attributable mortality cost; SAMes represents smoking-attributable mortality and PVLE is the present value of lifetime earnings.
Findings
Our study found that the economic cost of smoking for the entire population of Indonesia in 2019 ranged from Rp 184.36 trillion to Rp 410.76 trillion (see table 1). This research found a relatively similar number of the economic cost of smoking for the entire population (Rp 410.76 trillion, 2.59% of GDP) as compared with the previous estimate conducted by Kosen et al 10 at Rp 438.5 trillion (in the 2019 price), when using similar RR (from the USA) and GDP per capita as a proxy for income. The significant difference between the cost of smoking for those 20 years and older and the total population was the difference in the mortality cost of premature death.
The economic cost of smoking in Indonesia based on RRs from the USA and India, 2019 (Rp trillion)
Direct healthcare expenditure
The estimated direct cost of smoking in Indonesia for the total population ranges between Rp 17.9 and Rp 27.7 trillion, depending on the assumed RR (tables 2 and 3). Most of this cost (between 56.3% and 58.6%) is covered by BPJS-K. Inpatient and referral treatments make up its major component, representing between 86.3% and 87.6% of the cost to BPJS-K. The estimated cost for the population of those aged 20 years and up is very similar, between Rp 17.7 and Rp 26.7 trillion. Similarly, the estimated burden to BPJS-K is between 56.9% and 58.9% of total direct healthcare expenditure, with inpatient and referral treatments representing between 95.4% and 96% of the cost to BPJS-K. In other words, BPJS-K allocated between Rp 10.4 trillion and Rp 15.6 trillion to cover the healthcare costs attributable to smoking, which represents between 61.2% and 91.8% of the 2019 deficit.
Direct cost of smoking-attributable diseases in Indonesia in 2019 (Rp billion), by using different RRs
Direct cost of smoking-attributable diseases in Indonesia in 2019 (Rp billion) for the total population, by using different RRs
Direct healthcare cost increases with the age of smokers and reaches the maximum in the 50–59 years age group, with the estimated cost between Rp 4.6 trillion and Rp 6.3 trillion (table 3). The direct healthcare expenditure per ever-smoker that should be covered by BPJS-K increases between 122% and 138% for individuals in the 50–59 years age group relative to younger age groups. The estimates based on the RR from the USA continue to rise, while the cost based on India RR remains stable after age 60 years.
The average per-person BPJS-K cost increases with the age of ever-smokers (table 4). Using the RR from the USA, the average BPJS-K cost per ever-smoker continues to increase with age. However, the RR from India shows a slight reduction of direct healthcare cost per ever-smokers for individuals in the 70+ years age group. The burden to BPJS-K to cover SDE for all populations is significantly higher than the estimated maximum allocation from the 2019 local cigarette tax and tobacco product excise tax sharing fund from the central government to local governments (Dana Bagi Hasil Cukai Hasil Tembakau (DBHCHT)-Revenue Sharing Fund of Tobacco Products Excise) for Indonesia’s healthcare system at only Rp 7.4 trillion (26.7% of the SDE).
Average per ever-smokers cost, 2019 (Rp), by using different RRs
Discussion and conclusion
How this study differs from previous studies
Kosen et al 10 used the loss of DALYs to quantify the sum of the years of life lost due to premature mortality and the years of healthy life lost due to disability due to smoking-attributable diseases. They used the proportion of attributable risks based on data from a US Surgeon General report and 1 997 385 cases of 33 smoking-related diseases in the 2013 RISKESDAS prevalence data, which they multiplied with Indonesia Case Base Groups rates per episode per case. They then estimated that the total productive years lost due to morbidity, disability and premature mortality in 2015 was 8 558 601 DALYs. With the GDP per capita of Indonesia in 2015 (IMF) at US$3362, the total macroeconomic loss was US$28.7 billion or equal to Rp 438.5 trillion (at the 2019 value).
This study differs from Kosen et al 10 in three main areas to make the estimate more realistic. First, this study estimates the inpatient utilisation and the number of days affected by illnesses for those not seeking inpatient treatment instead of using the annual cost to access treatment due to smoking-related illnesses in Kosen et al.10 This allows for the inclusion of costs from individuals who suffered from illnesses but decided not to seek treatment at healthcare facilities—a common occurrence in Indonesia. Indonesia has not yet reached universal healthcare coverage, and individuals registered as BPJS-K still face barriers to access medical treatment.
Second, this study covers a wider range of the economic costs of smoking by applying the RR from India rather than only from the USA to estimate SAF for Indonesia. By using the RR from India, a more realistic estimated cost is expected, given the similarity in demographic characteristics, lifestyle and smoking intensity between Indonesia and India. Third, despite using DALYs, as in the study by Kosen et al, this study uses a cost of illness approach, which takes human capital into consideration. In calculating indirect morbidity (productivity loss due to an individual’s illness) and mortality costs (a loss to the economy due to an individual’s premature death), this study perceives the ‘market value’ of an individual’s future contribution to production in society if they had continued to work in full health. So, our approach is designed to estimate the value of human capital at the present value of his or her future earnings. We used future earnings as a proxy for future productivity.
The bottom line for policy
This study confirms that the cost of smoking places a substantial burden on Indonesian society and the healthcare system and specifically puts JKN at risk of becoming an ever-larger strain on public finances as coverage grows. Without further intervention, the cost of smoking is expected to escalate due to the growing size of the population, mainly due to the rise of costs associated with chronic diseases attributable to smoking.
The 2020 tobacco excise tax policy was not sufficient to cover the costs of smoking as the government only allocated a small fraction of it for JKN. When we adjusted with inflation, the 2020 direct smoking cost is approximately Rp 18.2 to Rp 28.2 trillion (between 0.1% and 0.2% of the GDP). In the JKN scheme, the government pays a modest premium for the impoverished, which covers about 96.5 million individuals, a fraction of which is earmarked from the tobacco tax. Based on Presidential Regulation No. 82/2018, the government is mandated to allocate a fraction of the local cigarette tax for JKN. Although in 2020, the government received Rp 170.2 trillion in tobacco excise revenues (YOY (Year-Over-Year) growth of 3.3%), the allocation earmarked for JKN was only at a maximum of Rp 8.1 trillion (comprised Rp 6.4 trillion from the local cigarette tax and Rp 1.7 trillion from the revenue sharing of tobacco excise tax (DBHCHT).
As evidence from many countries shows, making cigarettes less affordable decreases the demand for tobacco products: it discourages non-users from taking up tobacco use, encourages existing users to reduce consumption or even to quit, helps former users maintain cessation and prevents occasional smokers from turning into regular smokers.20 22 Non-smokers are less likely than smokers to develop heart disease, stroke and lung cancer, and smokers who successfully quit before age 40 years avoid nearly all increased mortality risks attributable to continued smoking.23
Our study provides evidence for a stronger government policy to control tobacco consumption, or else the economy will lose economic productivity in the long term. A stronger tobacco control policy is necessary for Indonesia. This could be in the form of a tobacco tax increase, prohibition of cigarette advertisements in public spaces or stronger enforcement of designated smoking areas to reduce smoking behaviour.
Further study
This study has two main limitations. First, the study does not use RR from Indonesia because it is unavailable. Therefore, it employs RRs from the USA and India. Moreover, the RR of India is for mortality but is used to estimate the Indonesian population’s attributable morbidity. While many studies show no significant impact on using such estimates, this may be problematic if the risks of morbidity and mortality from tobacco use are significantly different. However, this approach has been widely used in the literature,16–18 and the use of RR of mortality as a proxy for RR of healthcare utilisation is expected to yield an underestimated and conservative SAF for medical costs.24
Second, the RR for the USA was estimated for the population aged 35 years or older, while the RR for India was 30–69 years of age. In contrast, this study estimates the cost for the total population aged 20 years and older. For that reason, when the US RR is used, the same RR for the 35–54 years age group is assumed for the population younger than 35 years, and in the case of India RR, the same RR is used for the population younger than 30 years. This is based on a strong assumption for these individuals and maybe an overestimation of the cost for these age groups.
What this paper adds
What is already known on this topic
A few attempts have been made to quantify the health and economic burden of smoking-related diseases in Indonesia.
The most recent estimate of the healthcare cost of smoking in Indonesia calculated only the cost to treat the primary diagnosis at the secondary and tertiary care levels (advanced care), resulting in underestimation.
Even though these costs fall mainly on the Social Security Agency for Health and negatively impact the National Health Insurance System (NHIS)’s sustainability, until this study, Indonesia did not have a reliable estimate of the direct cost of smoking born by NHIS.
What this study adds
Compared with previous studies, calculations in this study should result in more realistic estimates for policymaking.
The direct cost of smoking is higher than previously calculated and is well above the annual health budget.
The current tobacco excise tax policy is insufficient to cover the cost of smoking.
This study using the WHO standard approach provides a more comprehensive and realistic estimate of the healthcare cost of smoking in Indonesia by including all diseases and all levels of care.
This study also improves our understanding of the healthcare burden of tobacco use in low-income and middle-income countries while demonstrating the feasibility of conducting such studies in countries where resources and valid data are scarce.
How this study might affect research, practice or policy
The report recommends policy interventions to reduce the prevalence of smoking and earmark revenue from tobacco more effectively.
Data availability statement
Data are available on reasonable request.
Ethics statements
Patient consent for publication
Ethics approval
This study uses secondary statistical data and does not involve human and animal subjects; therefore, an ethical clearance may not be required. Nevertheless, we still applied for and received ethical clearance approval from the Faculty of Medicine, Universitas Indonesia (No. KET-840/UN2.F1/ETIK/PPM.00.02/2019).
Acknowledgments
The authors would like to thank BPJS-K (SSAH) for providing a valuable administrative data of healthcare costs for inpatient and outpatient disaggregated by age group and gender, and to Professor Frank J Chaloupka (UIC), Dr Rijo M Jhon (Rajagiri College of Social Sciences (RCSS), Dr Violeta Vulovic (UIC) and Dr Evan Blecher (WHO) for their valuable inputs, comments and suggestions for improving the article.
Supplementary materials
Supplementary Data
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.
Footnotes
Contributors YM, DN and TD: conceived and designed the experiments; performed the experiments; analysed and interpreted the data; wrote the paper. NNHWL: performed the experiments; analysed and interpreted the data; wrote the paper. TD is responsible for the overall content as the guarantor.
Funding CISDI is funded by the University of Illinois at Chicago’s (UIC) Institute for Health Research and Policy to conduct economic research on tobacco taxation in Indonesia. UIC is a partner of the Bloomberg Initiative to Reduce Tobacco Use.
Disclaimer The views expressed in this document cannot be attributed to, nor do they represent, the views of UIC, the Institute for Health Research and Policy or Bloomberg Philanthropies.
Competing interests None declared.
Provenance and peer review Not commissioned; externally peer reviewed.
Supplemental material This content has been supplied by the author(s). It has not been vetted by BMJ Publishing Group Limited (BMJ) and may not have been peer-reviewed. Any opinions or recommendations discussed are solely those of the author(s) and are not endorsed by BMJ. BMJ disclaims all liability and responsibility arising from any reliance placed on the content. Where the content includes any translated material, BMJ does not warrant the accuracy and reliability of the translations (including but not limited to local regulations, clinical guidelines, terminology, drug names and drug dosages), and is not responsible for any error and/or omissions arising from translation and adaptation or otherwise.


