Abstract
Rationale
A network meta-analysis of randomized trials and real-world comparative studies strongly suggest that varenicline is more effective in aiding smoking cessation than single form nicotine replacement therapy (NRT). Modeling the health benefits attributable to this difference relies on extrapolation to lifetime cessation, but to date, follow-up has only extended to 12 months. Longer term follow-up data are helpful in checking these assumptions.
Objectives
This study aimed to compare the sustained abstinence rates of smokers using varenicline versus nicotine patch in their quit attempt up to 36 months.
Method
Five hundred eighty-seven smokers were recruited at Kaohsiung Veteran General Hospital between Feb 2006 and Aug 2009. Participants received counseling from a physician and received either varenicline (N = 296) or the nicotine patch (N = 291) for smoking cessation. Both varenicline and nicotine patch users could receive their medications for a maximum of 8 weeks. Participants were followed up by telephone at 3, 6, 12, and 36 months from the first visit. The primary outcome measure was self-reported sustained abstinence up to 36 months. Measures were also taken of smoking characteristics, cigarette dependence, and sociodemographic characteristics.
Results
Multiple logistic regression of 36-month sustained abstinence on to medication adjusting for other baseline variables showed a significant advantage for varenicline, OR = 7.94 (95 % CI 1.87–33.74).
Conclusion
An 8-week course of varenicline appears to yield higher abstinence rate up to 3 years than a similar length course of nicotine transdermal patch in routine clinical practice where behavioral support is available.
Similar content being viewed by others
Introduction
Several smoking cessation medicines are approved for smoking cessation and used in a number of countries (Piné-Abata et al. 2013) including various forms of nicotine replacement therapy (NRT) and bupropion. The most recently approved medication is varenicline, a nicotine acetylcholine receptor partial agonist targeting the alpha4-beta2 receptor subtype. Meta-analyses indicate that varenicline is more effective than bupropion for smoking abstinence (Cahill et al. 2012), and a recent network meta-analysis of RCTs (Cahill et al. 2013) and a number of real-world comparative studies (Kralikova et al. 2013; Stapleton et al. 2008) strongly suggest that varenicline is more effective than single form NRT in routine clinical practice. Modeling the health benefits and cost-effectiveness of different treatments requires extrapolation to lifetime cessation (Stapleton and West 2012) but studies extending beyond 12 months are very rare, and to date, none of these has compared varenicline with NRT. It is helpful to check assumptions about relative relapse rates after 12 months. It is also helpful to establish the generalizability of findings to different cultures.
The present study examined whether smokers using varenicline would be more likely to still be abstinent 36 months after the quit date than those using nicotine transdermal patch in a real-world setting: a treatment facility in Taiwan.
Methods
Study participants and process
We analyzed data from 587 smokers who attended the Department of Family Medicine outpatient department at Kaohsiung Veteran General Hospital, Taiwan, for help to quit smoking, who started treatment between February 2006 and August 2009, and who used either varenicline or nicotine patch. Nicotine patch was available throughout the study period, and varenicline was available after August 2007. To be included in this study, participants had to be 18 years or older, choosing either varenicline or nicotine patch in their quit attempt, and either smoking ≥10 cigarettes per day (CPD) or have a score of ≥4 on the Fagerström Test for Cigarette Dependence (FTCD) (Heatherton et al. 1991). They were excluded from the study if they were pregnant, used more than one form of stop-smoking medication, or had an unstable medical or mental health condition as assessed by the physician.
The cost of therapy for all patients was partially covered by Taiwan’s National Insurance Program. Both the nicotine patch and varenicline were subsidized NT$250Footnote 1 (approximately US$8.30 or 5.60€) per week. Participants needed to pay NT$545 (approximately US$18.2) per week for the nicotine patch and NT$746–984 (approximately US$24.9–32.8) per week for varenicline 0.5 mg/1 mg. The study was approved by the Ethics Review Committee of Kaohsiung Veterans General Hospital.
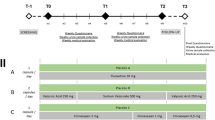
At the first visit, each smoker received 15–20 min with a physician, educational materials explaining smoking cessation techniques, and a prescription for either varenicline or the nicotine patch. Participants were instructed to try to stop smoking as soon as they started to use the patch. Varenicline users were instructed to set their quit day on the 8th day after starting the medication. A 1- to 2-week supply of medicine was prescribed at each of the clinic visits. Both nicotine patch and varenicline users could receive their medications for a maximum of 8 weeks. During the treatment, physicians were allowed to adjust the nicotine patch and varenicline dosage if patients experienced unacceptable side effects. However, most adverse events were mild to moderate and well tolerated in both groups.
After the first visit, patients were encouraged, but not required, to consult the clinic physician every 1 to 2 weeks to a maximum of eight visits in the following 90 days. After the first visit, each physician counseling session lasted up to 10 min. The content of the counseling provided depended on their physical dependence, withdrawal symptoms, drug adverse events, and their perceived barriers to quitting. If the patient did not attend one of the follow-up visits, they would not receive a prescription for the drug they were taking. The clients were followed up by telephone at 3, 6, 12, and 36 months.
Data collection and outcome measure
At the first visit, each patient completed a questionnaire collecting demographic information and data related to smoking status, cigarette dependence level (measured using the FTCD), and expired air carbon monoxide (CO) concentration (ppm) and received their choice of smoking cessation medication. During subsequent visits, physicians collected data on withdrawal symptoms, drug adverse events, and difficulties they were encountering.
The primary outcome measure was self-reported sustained abstinence up to 36 months. All participants were contacted by telephone and asked about their smoking at 3, 6, 12, and 36 months after the first visit. They were asked “Are you smoking now?” (“Yes” or “No”) and “How many days is it since you smoked your last cigarette?” (“less than 24 h,” “1–7 days,” “8–30 days,” “30–90 days,” “90–180 days,” “180–365 days,” “more than 365 days,” and “unknown or forgot”). To be qualified as a quitter, participants must have answered “no” to the first question, at least 90 days’ abstinence at 3 months, at least 180 days’ abstinence at 6 months, at least 365 days’ abstinence at 12 months, and more than 365 days’ abstinence at 36 months. Any other pattern of responses led to the participant being regarded as a smoker and all those lost to follow-up were counted as smokers. Three call attempts were made at each follow-up.
If a patient was discovered to have died in the course of a follow-up, this was recorded.
Statistical analysis
The primary statistical analysis was a multiple logistic regression of sustained abstinence to 36 months on to medication choice (varenicline or nicotine patch) adjusting for other variables assessed at baseline. Because varenicline was not available from the start of the study period, we introduced a dummy variable coded as 0 before varenicline was introduced and 1 afterwards. The multiple regression included this variable. In addition, the shape of the relapse curve was plotted for both groups, and relapse rates were assessed from each follow-up point up to 36 months.
Results
Table 1 shows a summary of baseline characteristics of the sample. Compared with participants in patch group, those using varenicline had significantly higher FTCD scores (p < 0.001), educational level (p = 0.001), and smoked more cigarettes daily (p = .002).
Three patients in the NRT group died during the follow-up period and two in the varenicline group. In no cases did the death occur during the medication period, and the patients had previously failed to satisfy the abstinence criterion. Table 2 shows associations between baseline variables and 36-month abstinence. In the adjusted model, only educational level predicted outcome.
Table 3 shows the unadjusted and adjusted odds of abstinence up to each follow-up point. Clients who received varenicline were more likely to remain abstinent up to 36 months and every follow-up point prior to that. Adjusting for baseline variables increased the size of the odds ratios. This was because after varenicline was introduced into the clinic, the success rate of patients on NRT dropped while the success rate of those on varenicline were approximately double what the clinic had experienced prior to its introduction (Table 4). The success rate on varenicline was higher than the concurrent success rate in patients choosing NRT and the historic rate of those for whom NRT was the only option. The overall success rate of the clinic following introduction of varenicline was consequently higher than before varenicline was introduced.
Figure 1 plots the sustained abstinence rates in each medication group at each follow-up. The relapse curve after 3 months follows a similar trajectory with the exception of an upward deviation in the NRT group at 6 months. However, because the varenicline group started with a higher abstinence rate at 3 months, this means that they had a slightly lower relapse rate between then and 36 months (Table 5). The odds of relapse between 3 months and 36 months were non-significantly higher for the NRT group than the varenicline group (OR = 1.68, p = 0.12).
Discussion
This study confirms previous research showing that smokers who use varenicline rather than nicotine patch have a greater chance of stopping successfully. It extends these findings to a new population in a real-world setting and shows that the effect remains undiminished at 36 months. It also shows that the benefit occurs when the dosing period for varenicline and nicotine patch are 8 weeks.
Previous research has shown that combination NRT (typically transdermal patch plus a faster acting form) is more effective than single form. It remains to be seen whether varenciline is more effective long term than combination NRT (Cahill et al. 2012), but findings from a recent study in routine clinical practice suggest that any difference is likely to be small (Brose et al. 2013). There is also a suggestion that starting nicotine patches prior to the quit date may improve success rates (Cahill et al. 2012), and this too may reduce or eliminate the difference in effectiveness between NRT and varenicline.
The fact that the relapse rates following treatment were similar in the two conditions is in line with previous research which has found that smoking cessation treatments have lasting effects by boosting the numbers of users who achieve short-term abstinence, and with similar relapse rates following this, the relative success rate is sustained even though the absolute rate diminishes.
Our study had several limitations. First, this was a cohort study where varenicline was not available in the first period of recruitment, and patients could choose between varenicline and NRT in the second period. Therefore, there were opportunities for undetected bias. A secular trend in success rates is unlikely to explain the findings because adjusting for pre- versus post-introduction of varenicline to the clinic increased the effect size. In fact, the opportunity to compare varenicline success rates with NRT when patients could choose either and NRT before a choice was available rules out both secular trend and patient choice as factors. The picture is further clarified by the fact that the success rates of the entire clinic increased once varenicline was introduced, and this was wholly attributable to higher success rates in those on varenicline.
It is noteworthy that educational level of those choosing varenicline was higher, but adjusting for this made minimal difference to the effect size, and in any case, FTCD scores, normally predictive of relapse or lapse (Sweitzer et al. 2013), were higher in this group. It is possible that other unobserved variables such as the mental health status of those on varenicline was better and this may have contributed to the difference, but other real-world studies have been able to adjust for this and obtained broadly similar effect sizes (Kralikova et al. 2013).
Another limitation is that participants were contacted by phone to collect information on their self-reported abstinence rates at 3, 6, 12, and 36 months without biochemical validation; however, there is no reason to believe that the participants would differ in rate of misreporting of smoking status as a function of their medication choice. Lastly, it may be argued that having to pay more for their medication led to those on varenicline being more motivated to remain abstinent. However, other research has found that paying for stop-smoking medication has the reverse effect, reducing adherence and success rates (Kaper et al. 2005).
The fact that the relapse rate after 3 months was at least as high, and possibly higher, in those patients using NRT indicates that the effect of varenicline does not dissipate in the long term. The relapse rates were within the expected range from studies involving other treatments (Stapleton et al. 1998).
The failure of the FTCD to predict abstinence has been found in several other studies in non-English speaking populations (Wee et al. 2011a; Wee et al. b). In this case, it could have been due to the fact that all patients were receiving pharmacotherapy or that patients were only eligible for treatment if they had a relatively high FTCD score.
The fact that educational level predicted outcome to 36 weeks confirms the importance of this variable cross-culturally (Vangeli et al. 2011). There is an important research agenda in determining what underlies this so that treatment methods can target this source of health disparity.
In conclusion, findings from this study support the hypothesis that there is an advantage of varenicline over nicotine patch on long-term cessation rates in the context of a behavioral support program.
Notes
NT$ Taiwanese dollar
References
Brose LS, West R, Stapleton JA (2013) Comparison of the effectiveness of varenicline and combination nicotine replacement therapy for smoking cessation in clinical practice. Mayo Clin Proc 88(3):226–233. doi:10.1016/j.mayocp.2012.11.013
Cahill K, Stead LF, Lancaster T (2012) Nicotine receptor partial agonists for smoking cessation. Cochrane Database Syst Rev 4, CD006103. doi:10.1002/14651858.CD006103.pub6
Cahill K, Stevens S, Perera R, Lancaster T (2013) Pharmacological interventions for smoking cessation: an overview and network meta-analysis. Cochrane Database Syst Rev 5, CD009329. doi:10.1002/14651858.CD009329.pub2
Heatherton TF, Kozlowski LT, Frecker RC, Fagerstrom KO (1991) The Fagerstrom test for nicotine dependence: a revision of the Fagerstrom Tolerance Questionnaire. Br J Addict 86(9):1119–1127
Kaper J, Wagena EJ, Willemsen MC, van Schayck CP (2005) Reimbursement for smoking cessation treatment may double the abstinence rate: results of a randomized trial. Addiction 100(7):1012–1020. doi:10.1111/j.1360-0443.2005.01097.x
Kralikova E, Kmetova A, Stepankova L, Zvolska K, Davis R, West R (2013) Fifty-two-week continuous abstinence rates of smokers being treated with varenicline versus nicotine replacement therapy. Addiction. doi:10.1111/add.12219
Piné-Abata H, McNeill A, Murray R, Bitton A, Rigotti N, Raw M (2013) A survey of tobacco dependence treatment services in 121 countries. Addiction. doi:10.1111/add.12172
Stapleton JA, West R (2012) A direct method and ICER tables for the estimation of the cost-effectiveness of smoking cessation interventions in general populations: application to a new cytisine trial and other examples. Nicotine Tob Res 14(4):463–471. doi:10.1093/ntr/ntr236
Stapleton JA, Sutherland G, Russell MA (1998) How much does relapse after one year erode effectiveness of smoking cessation treatments? Long-term follow up of randomised trial of nicotine nasal spray. BMJ 316(7134):830–831
Stapleton JA, Watson L, Spirling LI, Smith R, Milbrandt A, Ratcliffe M, Sutherland G (2008) Varenicline in the routine treatment of tobacco dependence: a pre-post comparison with nicotine replacement therapy and an evaluation in those with mental illness. Addiction 103(1):146–154
Sweitzer MM, Denlinger RL, Donny EC (2013) Dependence and withdrawal-induced craving predict abstinence in an incentive-based model of smoking relapse. Nicotine Tob Res 15(1):36–43. doi:10.1093/ntr/nts080
Vangeli E, Stapleton J, Smit ES, Borland R, West R (2011) Predictors of attempts to stop smoking and their success in adult general population samples: a systematic review. Addiction 106(12):2110–2121. doi:10.1111/j.1360-0443.2011.03565.x
Wee LH, Shahab L, Bulgiba A, West R (2011a) Stop smoking clinics in Malaysia: characteristics of attendees and predictors of success. Addict Behav 36(4):400–403. doi:10.1016/j.addbeh.2010.11.011
Wee LH, West R, Bulgiba A, Shahab L (2011b) Predictors of 3-month abstinence in smokers attending stop-smoking clinics in Malaysia. Nicotine Tob Res 13(2):151–156. doi:10.1093/ntr/ntq221
Conflict of interest
RW and AM undertake research and consultancy for companies that manufacture smoking cessation products including nicotine replacement products and varenicline.
Funding
The authors disclosed receipt of the following financial support for the research and/or authorship of this article: Kaohsiung Veteran General Hospital (Grant numbers VGHKS98-CT3-07, VGHKS99-CT3-02). Robert West and Andy McEwen are funded by Cancer Research UK. Robert West is a member of the UK Centre for Tobacco and Alcohol Studies.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hsueh, KC., Hsueh, SC., Chou, MY. et al. Varenicline versus transdermal nicotine patch: a 3-year follow-up in a smoking cessation clinic in Taiwan. Psychopharmacology 231, 2819–2823 (2014). https://doi.org/10.1007/s00213-014-3482-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-014-3482-9